The patient was urgently referred to the dermatology department for clinical evaluation of mysterious skin lesions. Upon examination, the medical team advised the immediate discontinuation of a recently prescribed medication. A comprehensive diagnostic workup was initiated, including a skin biopsy and a battery of blood tests comprising a complete blood count, antibody screening, lupus anticoagulant testing, and various serology panels. As an initial therapeutic measure, the patient was prescribed oral corticosteroids.
Within twenty-four to forty-eight hours of starting the treatment, the intensity of the lesions significantly diminished, and the associated pain subsided. The laboratory results revealed leukocytosis accompanied by neutrophilia, while the antibody and lupus anticoagulant tests returned positive; however, the remaining serology results were negative. Twenty days later, the pathology report confirmed the definitive diagnosis of Sweet syndrome.
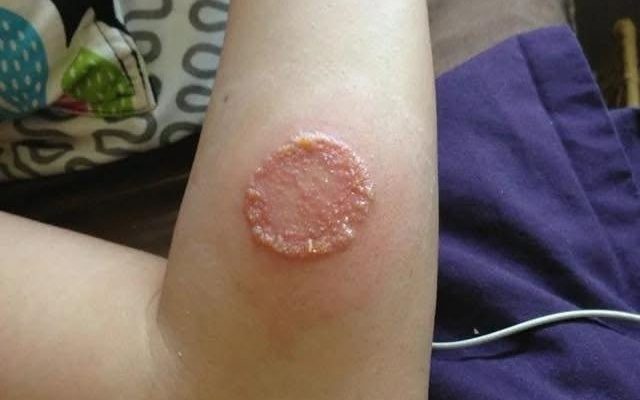
Sweet syndrome, also clinically recognized as acute febrile neutrophilic dermatosis, is a dermatological condition categorized under neutrophilic dermatoses. It is defined histopathologically by the presence of dense neutrophil infiltrates within the skin tissue. Clinically, the syndrome manifests as the sudden onset of painful, erythematous papules or plaques that are typically distributed bilaterally and asymmetrically. These lesions most commonly affect the face, neck, upper trunk, and hands. The condition is further characterized by systemic symptoms, including fever and leukocytosis with neutrophilia.
While the exact etiology of Sweet syndrome remains uncertain, scientific consensus suggests that its pathogenesis is mediated by cytokines that trigger the chemotaxis and activation of neutrophils and histiocytes. It is presumed to be a hypersensitivity reaction often preceded by an upper respiratory tract infection, the presence of paraneoplastic processes, or the intake of specific medications. Establishing a diagnosis is critical, as it necessitates the exclusion of underlying systemic diseases, particularly because atypical presentations of Sweet syndrome on the backs of the hands can serve as an early indicator of occult malignancy.
The condition is observed more frequently in women, particularly in cases classified as idiopathic or drug-induced. While common triggers are associated with contraceptives, antiepileptics, antibiotics, antihypertensives, colony-stimulating factors, and vaccines, other medications have also been linked to the onset of the syndrome, as evidenced by this specific clinical case.
The first-line pharmacological treatment for Sweet syndrome is oral corticosteroids, to which patients typically respond with remarkable speed. In most cases, general discomfort and pain recede within the first few hours of treatment, with cutaneous lesions resolving in less than a week. In this instance, the sudden onset of erythematous papular lesions on the face and neck required an extensive differential diagnosis, initially considering urticaria, contact dermatitis, toxicoderma, and cutaneous lupus. Following the systematic exclusion of these conditions through clinical history and complementary testing—and underscored by the conclusive biopsy results—the diagnosis of Sweet syndrome was confirmed.