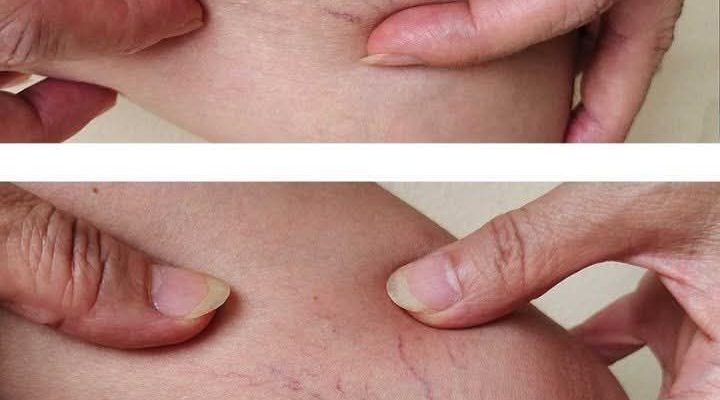
Noticing Red Veins on Your Thighs …Here’s What They Could Mean
Seeing thin red or purple veins spreading across your thighs can be unsettling — especially if your doctor’s appointment is still weeks away.
These visible lines are commonly called spider veins, medically known as telangiectasias. They’re small, dilated blood vessels that sit close to the surface of the skin, often forming web-like or branching patterns.
The good news?
They’re usually harmless.
But they can sometimes cause mild discomfort — and in certain cases, they may signal underlying vein issues worth monitoring.
Let’s break down what’s happening and what you can do right now.
What Causes Spider Veins?
Spider veins develop when tiny valves inside your veins weaken or become damaged. Normally, these valves keep blood flowing upward toward the heart. When they don’t function properly, blood can pool, causing veins to enlarge and become visible.
Several common factors increase your risk:
Genetics – A family history makes you more prone to developing them.
Hormonal changes – Pregnancy, menopause, or hormone therapy can affect vein strength.
Prolonged sitting or standing – Long hours at a desk or on your feet strain leg veins.
Obesity – Extra weight increases pressure on the venous system.
Sun exposure – UV damage can weaken small surface veins, especially in fair skin.
While many people experience no symptoms, some report:
Mild aching
Burning sensations
Itching
Heaviness in the legs after long periods of standing
What You Can Do Right Now
If you’re waiting to see a doctor, there are simple, low-risk steps you can take to ease discomfort and support healthy circulation.
- Elevate Your Legs
Raise your legs above heart level for 15–20 minutes a few times per day. This helps reduce venous pressure and encourages blood flow back toward the heart. - Wear Compression Stockings
Compression stockings gently squeeze the legs to improve circulation and reduce swelling. They’re especially helpful if your daily routine involves long periods of sitting or standing. - Keep Moving
Avoid staying in one position too long.
Take short walks.
Stretch every 30 minutes.
Flex your ankles if seated for extended periods.
Movement activates your calf muscles, which act as a natural pump for your veins.
- Apply Cold Compresses
Cold can temporarily reduce inflammation and soothe aching areas. - Gentle Massage
Light massage may stimulate circulation, but avoid deep pressure directly over visible veins.
Lifestyle Changes That Help Prevent More Spider Veins
Long-term prevention often comes down to daily habits.
✔ Stay Active
Low-impact exercises like walking, swimming, and cycling strengthen leg muscles and improve circulation without overstraining veins.
✔ Eat for Vein Health
Increase fiber to prevent constipation (which raises venous pressure).
Reduce salt to minimize water retention and swelling.
✔ Maintain a Healthy Weight
Less pressure on your legs means less strain on your veins.
✔ Protect Your Skin From the Sun
Apply sunscreen to your legs if they’re frequently exposed. UV damage can weaken delicate surface vessels.
✔ Avoid Tight Clothing
Clothing that constricts around the waist, groin, or legs can interfere with healthy blood flow.
Do Over-the-Counter Treatments Work?
Some non-prescription options may provide mild improvement in appearance or discomfort:
Topical creams with vitamin K or retinoids may strengthen small vessels over time.
Horse chestnut extract is sometimes used to support vein health.
Arnica gel may reduce inflammation and soreness.
Always consult your healthcare provider before starting supplements, especially if you take blood thinners or other medications.
When to Call Your Doctor Sooner
While spider veins are typically cosmetic, seek medical attention if you notice:
Persistent or worsening pain
Significant swelling
Skin ulcers or open sores
Bleeding from a vein
Rapid spread or sudden increase in visible veins
These symptoms could indicate deeper venous problems that require evaluation.
Final Thoughts
Spider veins can feel alarming when they first appear — but in most cases, they’re a common and manageable condition.
By supporting circulation, staying active, and adopting small lifestyle adjustments, you can often ease symptoms and reduce progression while waiting for professional guidance.
And remember: visible veins don’t automatically mean something serious — but paying attention to changes in your body is always a smart move.