Athlete’s Foot and Fungal Infections: Causes, Symptoms, Diagnosis, Treatment, and Prevention
Fungal infections affecting the feet are among the most widespread skin conditions globally. One of the most common of these infections is athlete’s foot, medically referred to as tinea pedis. Despite its name, this condition does not affect athletes exclusively. It can develop in anyone who is exposed to warm, damp environments that encourage fungal growth.
Understanding how athlete’s foot develops, how to recognize its symptoms, and how to treat and prevent it is essential for maintaining healthy skin and avoiding complications. With proper care, most cases can be effectively managed and prevented from returning.
What Is Athlete’s Foot?
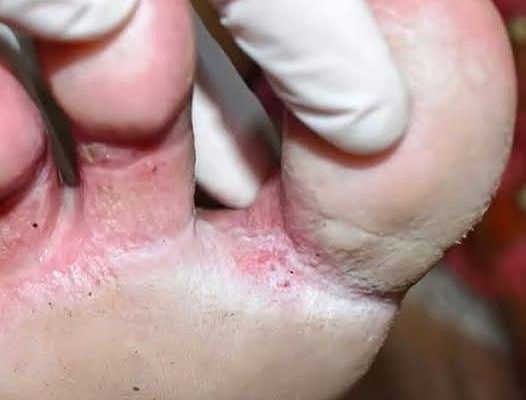
Athlete’s foot is a contagious fungal infection that primarily affects the skin of the feet, particularly the areas between the toes. It is caused by fungi known as dermatophytes, which feed on keratin—a protein found in the outer layer of the skin, as well as in hair and nails.
Dermatophytes thrive in warm, moist environments. This is why places such as locker rooms, communal showers, swimming pool areas, and even the inside of tight shoes can become ideal breeding grounds for fungal organisms. When the skin remains damp for extended periods, it becomes more susceptible to infection.
Although athlete’s foot is often associated with sports activities, anyone can develop it. Individuals who wear tight, non-breathable shoes, sweat excessively, or frequently walk barefoot in shared public spaces are at greater risk.
Causes of Athlete’s Foot
The infection is typically caused by dermatophyte fungi such as:
-
Trichophyton rubrum
-
Trichophyton interdigitale
-
Epidermophyton floccosum
These organisms invade the outer layer of the skin and multiply under favorable conditions. Fungi spread easily through direct skin-to-skin contact or indirectly through contaminated surfaces.
Common Risk Factors
Several factors increase the likelihood of developing athlete’s foot:
-
Wearing tight, closed-toe footwear for long hours
-
Failing to dry feet thoroughly after bathing or swimming
-
Walking barefoot in communal areas
-
Sharing socks, towels, or footwear
-
Excessive sweating (hyperhidrosis)
-
Living in warm, humid climates
-
Having a weakened immune system
Poor foot hygiene and prolonged moisture exposure create an environment in which fungi can flourish.
Signs and Symptoms
The symptoms of athlete’s foot can vary depending on the type and severity of the infection. Common signs include:
-
Persistent itching, especially between the toes
-
Burning or stinging sensations
-
Red, inflamed skin
-
Peeling or cracking skin
-
White, soggy skin between toes
-
Blisters or sores in severe cases
-
Dry, scaly patches on the soles or sides of the feet
-
Unpleasant foot odor
If untreated, the infection may spread to other areas of the body, including the toenails, hands, or groin. Nail involvement can lead to thickened, brittle, or discolored nails, which are more difficult to treat.
Different Forms of Athlete’s Foot
Athlete’s foot does not always appear the same. There are several recognized clinical patterns:
1. Interdigital (Toe Web) Type
This is the most common presentation. It typically affects the skin between the fourth and fifth toes. The area may appear moist, white, and peeling, and itching is often pronounced.
2. Moccasin-Type Infection
This form affects the soles and sides of the feet, creating a dry, scaly pattern that resembles the outline of a moccasin. The skin may become thickened, and nail involvement is more likely with this type.
3. Vesicular (Blistering) Type
Less common but more uncomfortable, this type involves fluid-filled blisters, usually on the soles. These blisters may be painful and can become secondarily infected if not properly treated.
How Athlete’s Foot Is Diagnosed
In many cases, a healthcare professional can diagnose athlete’s foot based on its appearance and symptom pattern. However, when the diagnosis is uncertain, additional tests may be performed.
Diagnostic Methods May Include:
-
Skin scraping and microscopic examination: A sample of skin is examined under a microscope to detect fungal elements.
-
Potassium hydroxide (KOH) test: Helps confirm the presence of fungi.
-
Fungal culture: Identifies the specific organism involved.
-
Wood’s lamp examination: In certain cases, ultraviolet light may help evaluate skin conditions.
These tests help distinguish athlete’s foot from other skin disorders such as eczema, psoriasis, or bacterial infections, which may require different treatments.
Treatment Options for Athlete’s Foot
Most mild cases respond well to over-the-counter antifungal treatments. More severe or persistent infections may require prescription medication.
1. Topical Antifungal Medications
Topical treatments are applied directly to the affected skin. Common options include:
-
Clotrimazole 1% cream
-
Miconazole nitrate
-
Terbinafine
-
Tolnaftate
-
Ketoconazole
These medications typically need to be applied for two to four weeks. Even if symptoms improve quickly, it is important to complete the recommended course to reduce the risk of recurrence.
2. Oral Antifungal Medications
In cases where the infection does not respond to topical treatments or spreads to the nails, a healthcare provider may prescribe oral antifungal medication. Examples include:
-
Oral terbinafine
-
Itraconazole
-
Fluconazole
Oral treatment may last several weeks. Medical supervision is important because some medications require monitoring for potential side effects.
3. Supportive Care Measures
In addition to medication, supportive measures are essential:
-
Keep feet clean and dry
-
Dry carefully between the toes
-
Change socks daily
-
Choose breathable footwear
-
Alternate shoes to allow complete drying
-
Use antifungal powders if prone to sweating
Combining medication with proper hygiene greatly improves treatment success.
Preventing Athlete’s Foot
Prevention plays a key role in reducing recurrence. Good foot hygiene and environmental awareness can significantly lower the risk.
Practical Prevention Strategies
-
Wash feet daily with soap and water
-
Dry thoroughly, especially between toes
-
Wear moisture-wicking socks
-
Avoid sharing personal items
-
Wear protective footwear in communal areas
-
Disinfect shoes periodically
-
Wash towels and socks in hot water
Allowing shoes to dry fully between uses is especially important, as damp interiors encourage fungal growth.
Possible Complications
Although athlete’s foot is usually mild, ignoring it can lead to complications:
Nail Fungal Infection (Onychomycosis)
Fungal infection may spread to the toenails, causing thickening, discoloration, and brittleness. Nail infections are more difficult to treat and often require prolonged therapy.
Secondary Bacterial Infection
Cracked or blistered skin may allow bacteria to enter, potentially leading to cellulitis—a deeper skin infection requiring medical treatment.
Spread to Other Body Areas
The infection can spread to the hands (tinea manuum) or groin (tinea cruris) through scratching or contact.
Increased Risk in Certain Individuals
People with diabetes, poor circulation, or weakened immune systems are at higher risk for complications. For these individuals, early medical evaluation is particularly important.
When to Seek Medical Advice
Consult a healthcare professional if:
-
Symptoms persist after two weeks of self-care
-
The infection spreads or worsens
-
Signs of bacterial infection appear (swelling, redness, pus)
-
You have diabetes or immune-related conditions
-
The infection involves the nails
Prompt treatment can prevent more serious problems and reduce the risk of spreading the infection.
Maintaining Long-Term Foot Health
Beyond treating active infections, maintaining overall foot health is essential. Regular inspection of the feet can help detect early changes. Keeping nails trimmed, managing excessive sweating, and selecting well-fitting shoes contribute to overall skin integrity.
For individuals prone to recurrent infections, preventive antifungal products may be used periodically under professional guidance. Lifestyle adjustments—such as alternating shoes and choosing breathable materials—can make a meaningful difference.
Conclusion
Athlete’s foot is a common yet manageable fungal infection that affects millions of people worldwide. Though often mild, it can cause discomfort and may lead to complications if left untreated. Fortunately, with early recognition, appropriate antifungal treatment, and consistent hygiene practices, most cases resolve successfully.
Preventive habits—such as keeping feet dry, wearing protective footwear in communal spaces, and avoiding shared personal items—are simple but highly effective strategies. By understanding the causes, symptoms, and treatments of athlete’s foot, individuals can protect their skin health and reduce the likelihood of recurrence.
With attentive care and timely action, healthy, comfortable feet are well within reach.